Journal Description
BioMed
BioMed
is an international, peer-reviewed, open access journal on the broad field of subjects in human life science and medicine published quarterly online by MDPI.
- Open Access— free for readers, with article processing charges (APC) paid by authors or their institutions.
- Rapid Publication: manuscripts are peer-reviewed and a first decision is provided to authors approximately 27 days after submission; acceptance to publication is undertaken in 6 days (median values for papers published in this journal in the second half of 2023).
- Recognition of Reviewers: APC discount vouchers, optional signed peer review, and reviewer names published annually in the journal.
- BioMed is a companion journal of Biomedicines.
subject
Imprint Information
Open Access
ISSN: 2673-8430
Latest Articles
Implementing A Flexible Sensor to Identify Forces during Instrument-Assisted Soft Tissue Mobilization
BioMed 2024, 4(2), 100-111; https://doi.org/10.3390/biomed4020008 - 16 Apr 2024
Abstract
►
Show Figures
Instrument-assisted soft tissue mobilization (IASTM) techniques use specialized hand-held instruments for applying controlled mechanical forces to the body with the goal of facilitating healing, improving range of motion, and reducing pain. Nevertheless, an optimal range of forces for achieving clinical outcomes has yet
[...] Read more.
Instrument-assisted soft tissue mobilization (IASTM) techniques use specialized hand-held instruments for applying controlled mechanical forces to the body with the goal of facilitating healing, improving range of motion, and reducing pain. Nevertheless, an optimal range of forces for achieving clinical outcomes has yet to be established. A barrier to advancing research on IASTM force optimization is the lack of commercially available instruments that quantify treatment forces. The aim of the current study was to assess the feasibility of attaching a flexible force sensor to a commercially available IASTM instrument to obtain valid force measurements. The validity of this novel approach was assessed by comparing data between the flexible force sensor and a force plate during a simulated treatment. Intraclass correlation coefficients, linear regression models, and Bland Altman plots all indicated excellent agreement between the force plate and flexible sensor when the instrument was used at 45°, 65°, and 90° treatment angles. Agreement between measures decreased when the instrument was held at 30°. Thus, commercially available instruments with attached sensors could make force measurement more accessible and feasible for a wider range of research settings, facilitating the advancement of IASTM research and ultimately informing clinical decision-making to improve patient care.
Full article
Open AccessArticle
Form Matters—Technical Cues in the Single Leg Heel Raise to Failure Test Significantly Change the Outcome: A Study of Convergent Validity in Australian Football Players
by
Brady Green, Molly Coventry, Tania Pizzari, Ebonie K. Rio and Myles C. Murphy
BioMed 2024, 4(2), 89-99; https://doi.org/10.3390/biomed4020007 - 07 Apr 2024
Abstract
►▼
Show Figures
Practitioners routinely use the single leg heel raise (SLHR) to quantify calf function in healthy and injured populations. Despite this, approaches vary and the impact of cueing on SLHR performance and results interpretation in athletesis unknown. The primary aim of this study was
[...] Read more.
Practitioners routinely use the single leg heel raise (SLHR) to quantify calf function in healthy and injured populations. Despite this, approaches vary and the impact of cueing on SLHR performance and results interpretation in athletesis unknown. The primary aim of this study was to quantify the level of agreement of the cued versus non-cued SLHR tests. The secondary aim was to explore test outcomes and the potential impact of intrinsic factors. Cued and non-cued SLHR tests were conducted in fifty-one Australian football players (23 women, 28 men). Metronome pacing (60 bpm) and five key cues were included in the cued condition. The level of agreement (Bland–Altman) between tests was measured for capacity (repetitions to failure) and asymmetry. Data from 100 legs were included. The non-cued and cued SLHR tests demonstrated poor agreement in both capacity and asymmetry. More repetitions to failure were performed in the non-cued SLHR [Mean (SD) = 33.9 (10.3) vs. 21.9 (5.3), p < 0.001)], and men had greater capacity (36.8 (10.4) vs. 30.3 (9.2), p < 0.001). During the cued SLHR, older players (age ≥ 30 years: −5.1 repetitions, p = 0.01) and Indigenous players (−3.4 repetitions, p = 0.002) and had reduced calf muscle function. Cueing the SLHR test significantly changes the result—outcomes are not comparable or interchangeable with the commonly used non-cued SLHR. These findings can guide practitioners quantifying calf capacity.
Full article
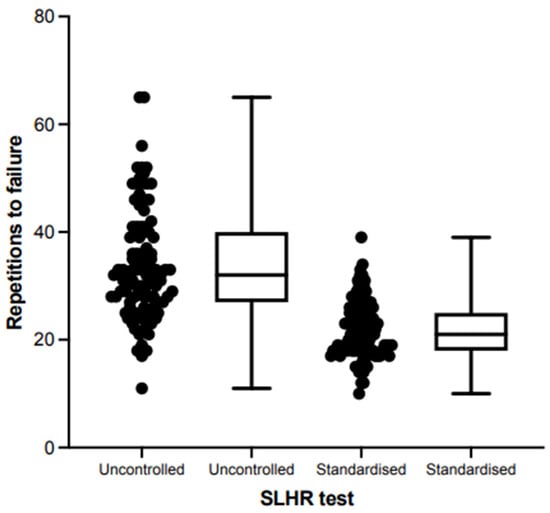
Figure 1
Open AccessArticle
Resilience and Sense of Coherence among Female Fibromyalgia Patients Living in a Conflict Zone Who Underwent Fibrotherapy Intervention
by
Liraz Cohen-Biton, Dan Buskila and Rachel Nissanholtz-Gannot
BioMed 2024, 4(2), 78-88; https://doi.org/10.3390/biomed4020006 - 22 Mar 2024
Abstract
►▼
Show Figures
Objective: This study sought to examine whether the sense of coherence (SoC) and resilience among female fibromyalgia (FM) patients increased after participation in a fibrotherapy intervention program (FTI) and whether SoC and resilience increased among female FM patients (FFMPs) exposed to security threats
[...] Read more.
Objective: This study sought to examine whether the sense of coherence (SoC) and resilience among female fibromyalgia (FM) patients increased after participation in a fibrotherapy intervention program (FTI) and whether SoC and resilience increased among female FM patients (FFMPs) exposed to security threats who changed their coping strategies to problem-oriented coping. Methods: Ninety-six FFMPs aged 19–75 enrolled in the FTI program led by Rabbi Firer in Sderot, Israel. The intervention program is divided into three stages, each comprising a distinct weekly treatment plan. The treatment plans encompass the following modalities: physiotherapy adapted to FM conditions, group therapy, hydrotherapy, horticultural therapy/cooking therapy, Pilates, pottery therapy, and kundalini yoga. Each stage spans a duration of 10 weeks, culminating in a total program duration of 30 weeks. Results: The findings show that after participating in FTI, the problem-orientation level of coping and health indicators, including functional ability and physiological scores (pre- and post-exertion), increased while psychological distress levels decreased. Overall, all the physiological scales measured before and after the FTI showed a significant improvement among the entire sample. FFMPs with problem-oriented strategies reported higher levels of SoC and resilience after participating in the FTI program. Conclusions: The FTI provided FFMPs with tools to understand the meaning of their disease and its management, whereas before they were preoccupied with the presence of the disease and its negative impact on their lives. The participation of FFMPs in the FTI leads to a perceptual change, the adoption of problem-oriented coping strategies, and the increased utilization of coping resources, namely, SoC and resilience. Problem-oriented coping combined with high SoC and resilience led FFMPs to adopt health strategies such as physical activity and other empowering activities that raised their physical and mental health indicators.
Full article
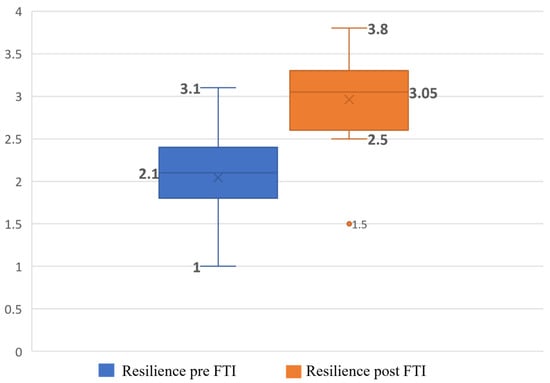
Figure 1
Open AccessArticle
Green Synthesis of Cocos nucifera-Based Nanomaterials and Mechanistic Basis of Their Antimicrobial Action
by
Zuriatou Yajeh Tanka, Naphtali Odogu Ankoro, Vincent Ngouana, Franklin Loïc Tchinda Taghu, Abongta Lum Mforbesi, Branly-Natalien Nguena-Dongue, Julius Nsami Ndi, Boniface Pone Kamdem, Paul Keilah Lunga and Fabrice Fekam Boyom
BioMed 2024, 4(1), 59-77; https://doi.org/10.3390/biomed4010005 - 06 Mar 2024
Abstract
Caused by pathogenic microorganisms, infectious diseases are known to cause high mortality rates, severe burdens of disability, and serious worldwide aftermaths. Drug-resistant pathogens have reduced the efficacy of available therapies against these diseases, thus accentuating the need to search for effective antimicrobials. Medicinal
[...] Read more.
Caused by pathogenic microorganisms, infectious diseases are known to cause high mortality rates, severe burdens of disability, and serious worldwide aftermaths. Drug-resistant pathogens have reduced the efficacy of available therapies against these diseases, thus accentuating the need to search for effective antimicrobials. Medicinal plants have served as starting material for the preparation of a number of antimicrobial agents. To this end, the present study highlights the green synthesis of Cocos nucifera-based nanomaterials and evaluation of the mechanistic basis of their antimicrobial action. Accordingly, Cocos nucifera extract was used for the reduction of silver nitrate solution to afford silver nanoparticles. These entities were further incorporated onto sulfuric-acid-based activated carbons to generate the nanocomposites. The antimicrobial activity of the as-prepared nanomaterials was evaluated using the broth microdilution method, while the antioxidant activity was assessed through standard methods. The cytotoxicity of potent nanomaterials was assessed on Vero cells by the spectrophotometric method. As a result, nanoparticles were successfully synthesized, as evidenced by the ultraviolet–visible spectroscopy analysis that revealed an intense absorption spectrum at 433 nm. Fourier Transform Infrared Spectroscopy presented the functional group moieties involved as a capping and reducing agent in the synthesis of the nanomaterials. The incubation of nanomaterials with selected bacterial and fungal strains has led to significant inhibitory effects of these pathogens with minimum inhibitory concentrations ranging from 7.813 to 250 μg/mL. In antioxidant assays, the nanocomposites presented scavenging activities comparable to those of ascorbic acid. Cytotoxicity experiment revealed no toxic effects on Vero cells (range of selectivity indices: from >4 to >128). These results provide evidence of the implication of Cocos nucifera-based nanomaterials in targeting bacterial or fungal systems that mediate free-radical damage or by inhibiting the oxidative damage caused by selected bacteria and fungi, the most susceptible being Escherichia coli and Candida albicans, respectively.
Full article
(This article belongs to the Topic Recent Advancement in Biotechnology and Drug Development Using Cutting-Edge Platforms)
►▼
Show Figures
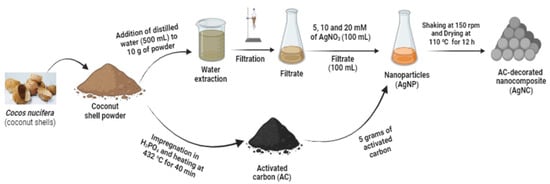
Figure 1
Open AccessArticle
Increased Risk for Non-Union in First Metatarsophalangeal Joint Arthrodesis following High-Velocity Reaming: A Retrospective Study
by
Assaf Albagli, Assaf Kadar, Ron Gurel, Elchanan Luger, Yaniv Warschawski and Shai Factor
BioMed 2024, 4(1), 50-58; https://doi.org/10.3390/biomed4010004 - 26 Feb 2024
Abstract
►▼
Show Figures
Objective: Arthrodesis of the first metatarsophalangeal joint (MTPJ) is a reliable procedure for treating various pathologies related to this joint. However, non-union is a common and debilitating complication of the procedure. The purpose of this study was to assess whether the use of
[...] Read more.
Objective: Arthrodesis of the first metatarsophalangeal joint (MTPJ) is a reliable procedure for treating various pathologies related to this joint. However, non-union is a common and debilitating complication of the procedure. The purpose of this study was to assess whether the use of a mechanical reamer to prepare the joint surface increases the risk of non-union compared to traditional manual osteotomy. Methods: A retrospective study of all patients who underwent their first MTPJ arthrodesis surgery in our medical center between 2010 and 2015. The articular surface preparation of the MTPJ was either manually performed (Group 1) or mechanically conducted with reamers (Group 2). Data regarding demographic characteristics, indications for surgery, osteosynthesis methods, and post-operative complications, including non-union, infection, and revision rates, were collected for all patients. Results: A total of 83 patients with 92 primary first MTPJ arthrodesis (44 cases in Group 1 and 48 cases in Group 2) were included with a mean follow-up time of 45.3 months (SD 16.8). The two groups were comparable in terms of age, gender, comorbidities, indication for surgery, and follow-up time. The non-union rate was 15.9% in Group 1 and 25% in Group 2 (p = 0.28). Group 2 showed a significantly higher rate of revision surgery compared to Group 1 (43.7% vs. 22.7%, p = 0.03). Conclusions: The mechanical reamer group had a higher non-union rate and a significantly higher rate of revision surgery compared to low-energy manual joint preparation. In light of these findings, the use of mechanical reamers for joint preparation in the first MTPJ arthrodesis was discontinued at our medical center.
Full article
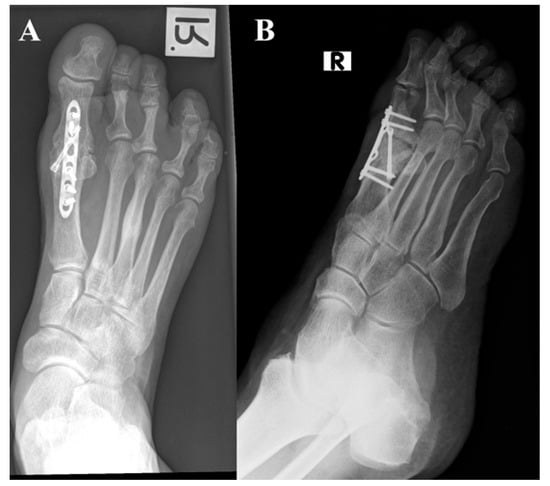
Figure 1
Open AccessArticle
Regular Intermittent Aerobic Exercise Reduces Arterial Stiffness Associated with Postprandial Hyperglycemia in Middle-Aged and Older Individuals
by
Ryota Kobayashi and Hideyuki Negoro
BioMed 2024, 4(1), 39-49; https://doi.org/10.3390/biomed4010003 - 08 Feb 2024
Abstract
►▼
Show Figures
Hardening of arterial walls associated with elevated postprandial blood glucose levels increases the risk of cardiovascular disease; however, the impact of intermittent aerobic training on reducing arterial stiffness is unknown. The aim of this study was to examine the chronic effects of intermittent
[...] Read more.
Hardening of arterial walls associated with elevated postprandial blood glucose levels increases the risk of cardiovascular disease; however, the impact of intermittent aerobic training on reducing arterial stiffness is unknown. The aim of this study was to examine the chronic effects of intermittent aerobic exercise on arterial stiffness during hyperglycemia in middle-aged adults: 30 healthy middle-aged adults were randomly assigned to an 8-week intermittent aerobic training group (n = 15, jogging or running, 30 min/run, 3 times/week, 65% reserve heart rate) and a control group (n = 15, no training). Pulse wave velocity (PWV) of carotid-femoral (cf) and brachial-ankle (ba), heart rate, blood pressure, and blood glucose was measured before a 75 g oral glucose tolerance test (OGTT) and 30, 60, and 90 min after the test, before the exercise intervention, and 4 and 8 weeks after intervention. The baPWV and blood glucose levels before the intervention were elevated at 30, 60, and 90 min in both groups compared to levels before the 75 g OGTT (p < 0.01). The baPWV and blood glucose levels after 4 and 8 weeks of intervention were unchanged in the training group compared to that before the 75 g OGTT, but increased at 30, 60, and 90 min in the control group compared to that before the 75 g OGTT (p < 0.01). The baPWV and blood glucose levels at 30 and 60 min after the 75 g OGTT after 4 and 8 weeks of intervention were lower in the training group than in the control group (p < 0.01). These results indicate that intermittent aerobic exercise training may reduce the acute increase in arterial stiffness after hyperglycemia.
Full article
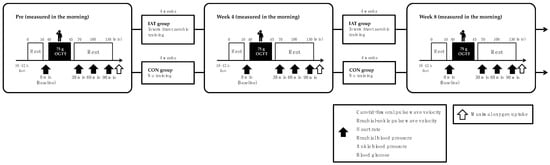
Figure 1
Open AccessReview
Complements from the Male Reproductive Tract: A Scoping Review
by
Rachel L. Washburn
BioMed 2024, 4(1), 19-38; https://doi.org/10.3390/biomed4010002 - 25 Jan 2024
Abstract
►▼
Show Figures
The organs of the male reproductive tract, including the testis, epididymis, prostate, seminal vesicles, and semen, must provide an immunoregulatory environment conducive to germ cell viability and successful fertilization. Many immune components, such as immune cells, have been investigated regarding reproductive immunology and
[...] Read more.
The organs of the male reproductive tract, including the testis, epididymis, prostate, seminal vesicles, and semen, must provide an immunoregulatory environment conducive to germ cell viability and successful fertilization. Many immune components, such as immune cells, have been investigated regarding reproductive immunology and function; however, the investigation of the role of complement in this system has only more recently been gaining traction in research. This review focuses on complement in the male reproductive tract, with the goal of compiling information currently known about complement components detected in male reproductive organs and identifying areas in need of further research. Considering the recent and upcoming research about the noncanonical functions of complement, this information is relevant and applicable in the fields of reproductive immunology, fertility, and immune regulation.
Full article
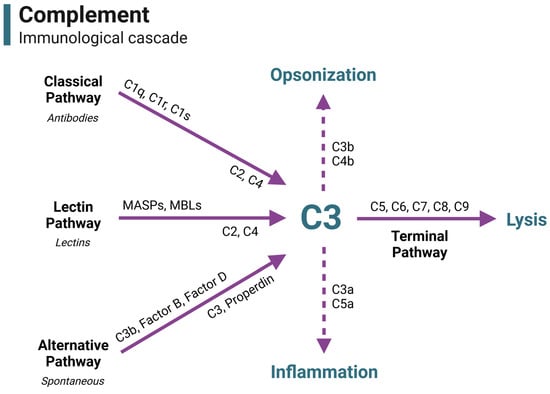
Figure 1
Open AccessReview
Oral Diseases and Adverse Pregnancy Outcomes in Sub-Saharan Africa: A Scoping Review
by
Ezekiel Taiwo Adebayo, Olunike Rebecca Abodunrin, Ifeoluwa E. Adewole, Abideen Olurotimi Salako, Joanne Lusher, Folahanmi Tomiwa Akinsolu, Maha El Tantawi, Omolola Titilayo Alade, George Uchenna Eleje, Oliver Chukwujekwu Ezechi and Moréniké Oluwátóyìn Foláyan
BioMed 2024, 4(1), 1-18; https://doi.org/10.3390/biomed4010001 - 29 Dec 2023
Abstract
►▼
Show Figures
This scoping review mapped and critically reviewed the extant literature exploring associations between oral disease status and adverse pregnancy outcomes among women residing in sub-Saharan Africa. A literature search was conducted in July 2023 using PubMed, Cochrane Library and Google Scholar. The articles
[...] Read more.
This scoping review mapped and critically reviewed the extant literature exploring associations between oral disease status and adverse pregnancy outcomes among women residing in sub-Saharan Africa. A literature search was conducted in July 2023 using PubMed, Cochrane Library and Google Scholar. The articles selected were those published in the English language between 1990 and 2022. After screening 833 potential studies, 15 articles met the inclusion criteria. Among these, 12 (80.0%) adopted a descriptive research design, while 3 (20.0%) used experimental methodologies. Eight (53.3%) studies were conducted in East Africa, fourteen (93.3%) studies were hospital-based, and one (6.7%) study was community-based. Periodontitis was linked with low birth weight, preterm birth, preterm birth and low birthweight, stunting, wasting, and underweight in most studies. Periodontitis was, however, not linked with adverse pregnancy outcomes in four studies. Caries was not linked with adverse pregnancy outcomes, but its sequalae was linked with low birth weight, preterm birth, neonatal stunting, and small head circumference. Two studies showed that periodontal diseases were linked with preeclampsia and chorioamnionitis. Maternal poor oral hygiene was linked with stunting. Two other studies showed no links between maternal periodontal disease and preterm premature rupture of membranes, eclampsia, spontaneous abortion, and vaginal bleeding. Furthermore, two intervention studies found that the treatment of periodontal diseases during pregnancy reduced the risk of adverse pregnancy outcomes. Further studies are needed to fully elucidate the effect size of the links observed between oral diseases and adverse pregnancy outcomes in sub-Saharan Africa.
Full article
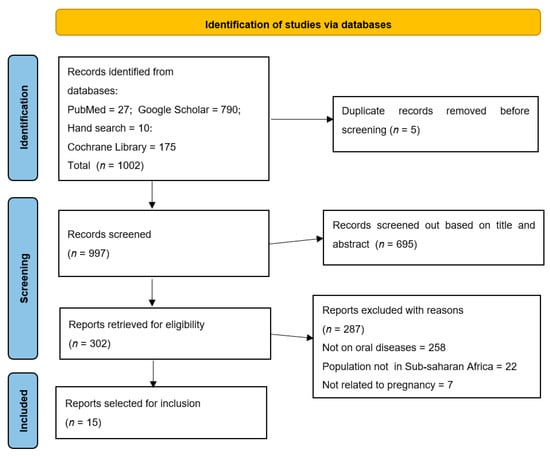
Figure 1
Open AccessArticle
Impacted Mandibular Third Molar Prevalence and Patterns in a Nigerian Teaching Hospital: A 5-Year Retrospective Study
by
Opeyemi Adeola, Olawunmi Fatusi, Azuka Njokanma and Adewale Adejobi
BioMed 2023, 3(4), 507-515; https://doi.org/10.3390/biomed3040040 - 21 Nov 2023
Abstract
Mandibular third molars are the most commonly impacted teeth. The prevalence and pattern of impacted mandibular third molars in patients presenting to the Obafemi Awolowo University Teaching Hospitals Complex, a tertiary hospital in south-western Nigeria, are largely unknown. This retrospective study examined 469
[...] Read more.
Mandibular third molars are the most commonly impacted teeth. The prevalence and pattern of impacted mandibular third molars in patients presenting to the Obafemi Awolowo University Teaching Hospitals Complex, a tertiary hospital in south-western Nigeria, are largely unknown. This retrospective study examined 469 patient records, extracting socio-demographic and clinical information for analysis. It also determined the prevalence and pattern of impacted mandibular third molars from January 2015 to December 2019. The positioning of impacted teeth was assessed via periapical radiographs utilizing Winter’s classification. Data were subjected to analysis with IBM SPSS version 20, utilizing frequencies, percentages, and likelihood ratios, with statistical significance set at p < 0.05. The prevalence of impacted mandibular third molars within the study cohort was 2.51%, with a higher incidence observed in the 21–29 age group (p < 0.001). Mesioangular impaction was the most prevalent, with pericoronitis being the primary reason for extraction, and periodontal pockets being the most common associated pathology.
Full article
(This article belongs to the Special Issue Psychosocial Factors and the Epidemiology of Oral Diseases)
Open AccessPerspective
Of Soldiers and Their Ghosts: Are We Ready for a Review of PTSD Evidence?
by
Adonis Sfera, Jonathan J. Anton, Hassan Imran, Zisis Kozlakidis, Carolina Klein and Carolina Osorio
BioMed 2023, 3(4), 484-506; https://doi.org/10.3390/biomed3040039 - 10 Nov 2023
Abstract
►▼
Show Figures
Psychosocial trauma has accompanied mankind since time immemorial and has been sufficiently portrayed in art and literature to suggest that posttraumatic stress disorder may be as old as combat itself. Since war is more frequent in human history than peace, public health measures
[...] Read more.
Psychosocial trauma has accompanied mankind since time immemorial and has been sufficiently portrayed in art and literature to suggest that posttraumatic stress disorder may be as old as combat itself. Since war is more frequent in human history than peace, public health measures are confined to mitigating the detrimental impact of battlefield experiences on combat participants. At present, PTSD outcome studies show mixed results, marked by high nonresponse rates, therapy dropout, and completed suicide, suggesting that novel strategies are urgently needed. Those of us who work routinely with combat veterans have noted an increasing trend of patients preferring mindfulness-based therapies as opposed to trauma-centered treatments, such as prolonged exposure or trauma-focused cognitive behavioral therapy. Preference for mindfulness over trauma-based therapies appears to coincide with the shift in research focus from the amygdala and fear to the insular cortex and interoceptive awareness. Therefore, rethinking PTSD as insular pathology is driven by the recent findings that neurons in this cortical area not only regulate cardiac rhythm but also record past intestinal inflammations. These discoveries likely explain the high comorbidity of stress-related disorders with premature endothelial senescence and a dysfunctional intestinal barrier. Moreover, the identification of the cholinergic anti-inflammatory pathway and the revelation that endothelial cells express alpha-7 nicotinic receptors has brought PTSD prevention and early detection within reach. In this narrative review, we discuss the relationship between early vascular aging, gut barrier disruption, and PTSD. We also examine the link between this pathology and faulty interoceptive awareness, surmising that hypertension and decreased heart rate variability are PTSD risk factors, while lipopolysaccharide, lipopolysaccharide binding protein, soluble CD14, microbial cell-free DNA, acyloxyacyl hydrolase, and IL22 comprise early detection markers of this disorder.
Full article
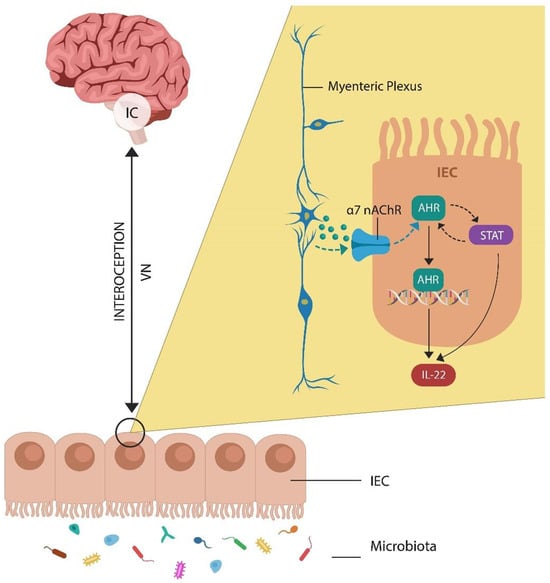
Figure 1
Open AccessArticle
Signs of Alveolar Collapse in Idiopathic Pulmonary Fibrosis, Hypersensitivity Pneumonitis and Systemic Sclerosis Revealed by Inspiration and Expiration Computed Tomography
by
Marco Fabian Wittwer, Soung-Yung Kim, Alexander Leichtle, Sabina Berezowska, Sabina A. Guler, Thomas Geiser, Johannes Heverhagen, Britta Maurer and Alexander Poellinger
BioMed 2023, 3(4), 471-483; https://doi.org/10.3390/biomed3040038 - 07 Nov 2023
Abstract
►▼
Show Figures
Idiopathic pulmonary fibrosis (IPF), hypersensitivity pneumonitis (HP) and systemic sclerosis (SSc) are among the most common entities that cause pulmonary fibrosis. Alveolar collapse with subsequent collapse induration of lung tissue is thought to contribute to the fibrotic transformation. The purpose of this study
[...] Read more.
Idiopathic pulmonary fibrosis (IPF), hypersensitivity pneumonitis (HP) and systemic sclerosis (SSc) are among the most common entities that cause pulmonary fibrosis. Alveolar collapse with subsequent collapse induration of lung tissue is thought to contribute to the fibrotic transformation. The purpose of this study was to examine lung tissue in computed tomography (CT) of non-diseased appearance during expiration for signs of increased density suggesting collapsibility in fibrosing lung diseases. We further analyzed the diaphragmatic movements during the respiratory cycle to determine relationships between density differences and the apex–diaphragm diameter. Significant differences in attenuation changes between inspiration and expiration of unaffected lung parenchyma were detected between IPF and controls and between HP and controls for all lung lobes (p < 0.001). Only minor differences were found between SSc and controls. There was no clinically relevant difference between patients with IPF and those with HP. The measured absolute apex–diaphragm diameter in inspiration and expiration demonstrated a statistically significant difference between patients with IPF versus normal controls. However, the diaphragmatic excursions were not different between these groups. Compared to controls, CT lung density increases significantly more during expiration in the fibrotic lungs of IPF and HP patients. The observed increase in density might indicate the collapse of alveoli during expiration and may represent a common pathophysiologic feature of fibrosing lung diseases. The density changes and lung extensions do not have the same ratios across different diseases and controls.
Full article
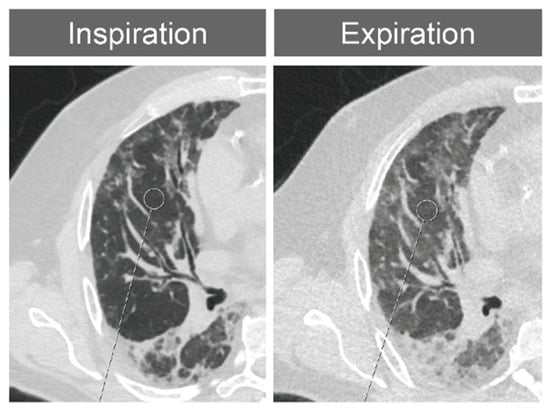
Figure 1
Open AccessReview
Relationships between Oral Health and the Sustainable Development Goals: A Scoping Review
by
Olunike Rebecca Abodunrin, Mobolaji Timothy Olagunju, Omolola Titilayo Alade and Morẹ́nikẹ́ Oluwátóyìn Foláyan
BioMed 2023, 3(4), 460-470; https://doi.org/10.3390/biomed3040037 - 30 Oct 2023
Cited by 1
Abstract
►▼
Show Figures
The aim of this scoping review was to map the research that links oral health and sustainable development goals (SDGs). The question that guided this review was what is the published evidence specifically linking oral health and SDGs? The search of articles published
[...] Read more.
The aim of this scoping review was to map the research that links oral health and sustainable development goals (SDGs). The question that guided this review was what is the published evidence specifically linking oral health and SDGs? The search of articles published between 2015 and June 2023 in English was conducted in June 2023 in PubMed, Web of Science, Cumulative Index to Nursing and Allied Health Literature, and Scopus. The extracted data from the 12 of the 520 publications that met the inclusion criteria were synthesized. These were publications from the African (n = 2) and European (n = 1) regions. Ten of the studies were not country specific. There were three observational studies. The referenced SDGs were SDG 1 (n = 1), SDG 3 (n = 11), SDG 4 (n = 3), SDG 5 (n = 2), and SDG 13 (n = 1). The studies linking oral health to SDG3 discussed a range of issues related to integrated oral health care, dental education on the SDGs, improved health equalities, access to universal health care, and sustainable health approaches. The small number of studies identified suggests the need to take proactive steps to generate research-based evidence that explores the interplay between oral diseases, oral health, and SDGs to address the dearth in the literature. By so doing, resources allocated to the SDGs can also be effectively uses to control oral diseases.
Full article
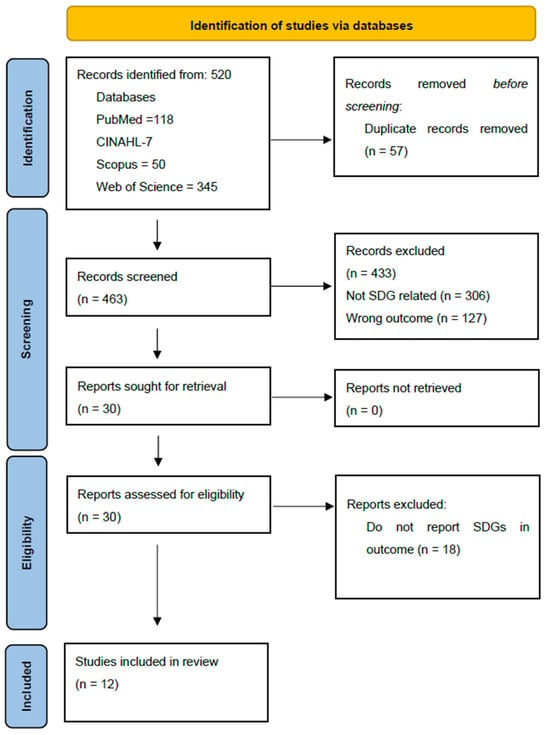
Figure 1
Open AccessArticle
Young vs. Old Population: Does Urban Environment of Skyscrapers Create Different Obesity Prevalence?
by
Yuval Arbel, Yifat Arbel, Amichai Kerner and Miryam Kerner
BioMed 2023, 3(4), 440-459; https://doi.org/10.3390/biomed3040036 - 24 Oct 2023
Abstract
►▼
Show Figures
This study investigates the impact of more densely populated urban environments proxied by the number of skyscrapers on the obesity prevalence among young vs. old populations at a US statewide level. Obesity is a global pandemic, as well as a major risk factor
[...] Read more.
This study investigates the impact of more densely populated urban environments proxied by the number of skyscrapers on the obesity prevalence among young vs. old populations at a US statewide level. Obesity is a global pandemic, as well as a major risk factor for a long series of health problems and increased mortality rates. We employ a quadratic model, which relaxes the a priori assumption of the monotonic rise or drop in obesity prevalence with the number of skyscrapers. The outcomes demonstrated a U-shaped curve and a sharper decrease (increase) in the projected obesity prevalence with the number of skyscrapers in the range of 0–147 (147–270) skyscrapers for the old population age cohorts above 65 years old. One possible explanation is the different motivation for physical activity among dissimilar age cohorts. While younger people are focused on maintaining a slim body shape, older people identify with the importance of sports. The public policy outcome of our study is the need to implement different recommendations in dissimilar urban environments based on age cohort stratification. Given that skyscrapers are the manifestation of wealth economics and present the typical characteristics of modern cities, which, in turn, are the future of economic development and productivity, these recommendations might prove to be important.
Full article
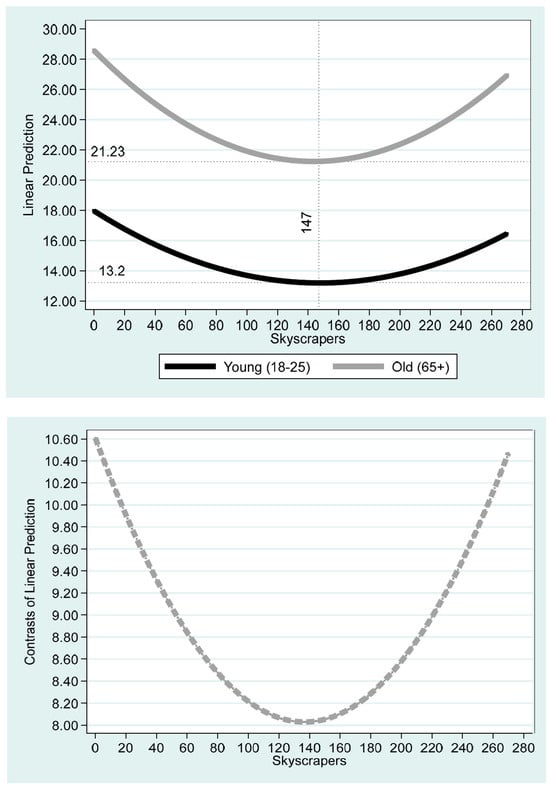
Figure 1
Open AccessOpinion
Untreated Early Childhood Caries and Possible Links with Brain Development
by
Morẹ́nikẹ́ Oluwátóyìn Foláyan, Omowumi Moromoke Femi-Akinlosotu, Bolu Adeoti and Oluwatosin Eunice Olorunmoteni
BioMed 2023, 3(4), 431-439; https://doi.org/10.3390/biomed3040035 - 28 Sep 2023
Cited by 1
Abstract
►▼
Show Figures
Untreated early childhood caries (ECC) is a global public health concern. In the short term, untreated ECC can lead to pain, infection, and disrupted sleep, among other issues. In the long term, it is associated with poor oral health in later life, increased
[...] Read more.
Untreated early childhood caries (ECC) is a global public health concern. In the short term, untreated ECC can lead to pain, infection, and disrupted sleep, among other issues. In the long term, it is associated with poor oral health in later life, increased risk of caries in permanent teeth, and adverse effects on physical and psychological development. There may be a link between untreated ECC and adverse cognitive and neurodevelopmental outcomes in young children, although the exact pathways are not fully understood. One possible pathway is through the relationship between mastication and brain stimulation. Impaired masticatory function due to ECC can affect the hippocampus, a key region responsible for memory and learning. Furthermore, untreated ECC can cause chronic inflammation, leading to the release of pro-inflammatory cytokines that may damage the brain. Sleep disturbances resulting from ECC-related pain and discomfort can also impact brain development and cognitive functioning. Additionally, frequent use of antibiotics and analgesics to address ECC-related infections can disrupt the gut microbiome, potentially affecting the brain through the gut–brain axis. Untreated ECC can cause nutritional deficiencies and elevated nutritional risk, and can further hinder brain development. Addressing ECC comprehensively with early childhood health initiatives can help mitigate potential long-term consequences and promote optimal brain development in young children.
Full article
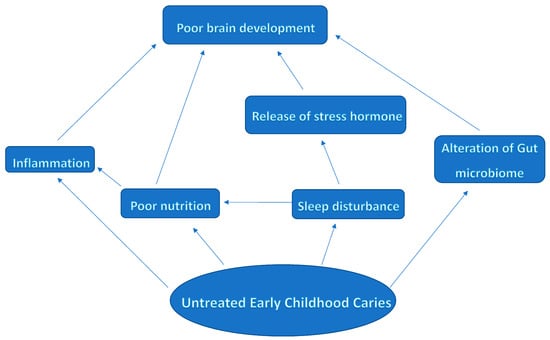
Figure 1
Open AccessArticle
HHV-6 in Cerebrospinal Fluid in Immunocompetent Children
by
Mikhail A. Nikolskiy, Dmitriy A. Lioznov, Evgeniy U. Gorelik and Tatyana V. Vishnevskaya
BioMed 2023, 3(3), 420-430; https://doi.org/10.3390/biomed3030034 - 20 Sep 2023
Abstract
►▼
Show Figures
Background: Human herpes virus-6 (HHV-6) is a ubiquitous virus known as an etiological agent of exanthem subitum. HHV-6-encephalitis in immunocompetent children is a rare complication of the primary infection. There are a lack of data on the prevalence of HHV-6-encephalitis in Russia. The
[...] Read more.
Background: Human herpes virus-6 (HHV-6) is a ubiquitous virus known as an etiological agent of exanthem subitum. HHV-6-encephalitis in immunocompetent children is a rare complication of the primary infection. There are a lack of data on the prevalence of HHV-6-encephalitis in Russia. The aim of our study was to analyze the prevalence of HHV-6 DNA in the cerebrospinal fluid (CSF) of immunocompetent children with suspected acute meningoencephalitis. Materials and Methods: A total of 712 CSF samples were tested using qualitative PCR over 12 years at N.F. Filatov Children’s City Clinical Hospital No.5, Saint-Petersburg, Russia. Results: HHV-6 DNA was detected in 20 (2.8%) of the samples. Retrospectively, we analyzed the medical records of 15 cases. There were seven boys and eight girls from 1 month to 7 years old; the mean age was 22.3 ± 5.6 months. Most HHV-6 DNA-positive cases were due to the primary form of HHV-6 infection. There were, in total, four cases of HHV-6-meningoencephalitis. All the children had a complete recovery, without neurological deficits or death. Conclusions: HHV-6 encephalitis is a very rare disease in immunocompetent children (four cases among 712 samples over 12 years). Additional studies are needed to develop accurate diagnostic criteria and therapeutic approaches.
Full article
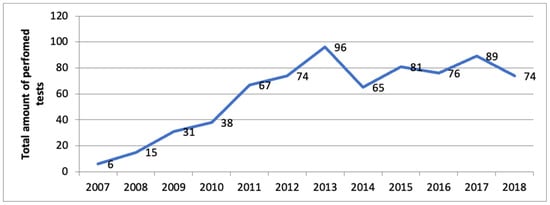
Figure 1
Open AccessReview
A Scoping Review of Early Childhood Caries Experience Assessment Tools Used for Studies in Nigeria
by
Adebola Oluyemisi Ehizele, Adebukunola Olajumoke Afolabi, Ukachi Chiwendu Nnawuihe, Omolola Titilayo Alade, Joanne Lusher, George Uchenna Eleje, Olunike Rebecca Abodunrin, Folahanmi Tomiwa Akinsolu, Ucheoma Nwaozuru, Maha El Tantawi, Morẹ́nikẹ́ Oluwátóyìn Foláyan and Francisca Obiageri Nwaokorie
BioMed 2023, 3(3), 400-419; https://doi.org/10.3390/biomed3030033 - 29 Aug 2023
Abstract
►▼
Show Figures
This scoping review provides an overview of the tools used to assess for early childhood caries (ECC) in Nigeria. A search of the literature in African Journals Online, Google Scholar, Medline, and Cochrane database was conducted in June 2023 using the PRISMA-ScR guidelines.
[...] Read more.
This scoping review provides an overview of the tools used to assess for early childhood caries (ECC) in Nigeria. A search of the literature in African Journals Online, Google Scholar, Medline, and Cochrane database was conducted in June 2023 using the PRISMA-ScR guidelines. A combination of keywords related to caries risk assessment, preschool children, and evaluation tools was used for the search. Studies reported in English and assessing ECC were extracted. Descriptive statistics were used to summarise the information on study characteristics, types of caries assessment tools, and study outcome. Caries assessment tools were divided into behavioural, social, and biological. After screening 964 potential studies, 16 were included in the review. ECC assessment tools were categorised into behavioural (snacking, frequency of consumption of refined carbohydrate in-between-meals, dental service utilisation, frequency of tooth brushing, use of fluoridated toothpaste, breast and bottle feeding patterns and duration), biological (birth rank, age, sex, anthropometric measures, molecular characterisation of isolated organisms, presence of plaque), and social (socioeconomic status of the child’s household, mother’s level of education, maternal income, occupation of the father, maternal decision-making ability). Twelve studies used behavioural assessment tools, 11 used biological, and 11 used social tools. Furthermore, 11 (70.1%) used a combination of tools, four (25.0%) used only biological tools, and one (6.2%) used only behavioural tools to assess ECC experience. No study screened for the risk of caries. In conclusion, we identified the need for comprehensive studies to identify the risk indicators of ECC in Nigeria. This will support the development of a caries risk assessment tool appropriate for the country context.
Full article
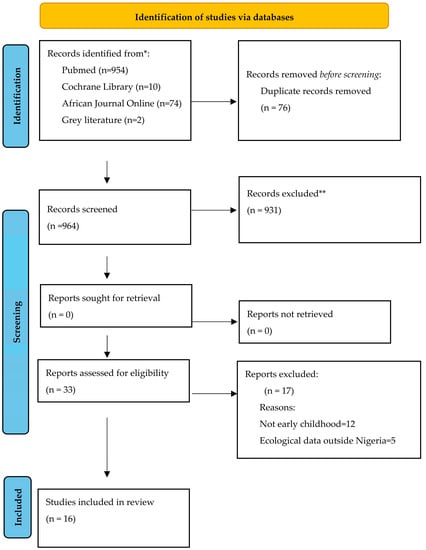
Figure 1
Open AccessCommunication
Decarbonization of Transport and Oral Health
by
Morenike Oluwatoyin Folayan and Maha El Tantawi
BioMed 2023, 3(3), 392-399; https://doi.org/10.3390/biomed3030032 - 16 Aug 2023
Abstract
The decarbonization of transport is a global initiative aimed at reducing greenhouse gas emissions and addressing the risks of global warming. This article explores the potential connections between the decarbonization of transport and oral health, highlighting the need for further research in this
[...] Read more.
The decarbonization of transport is a global initiative aimed at reducing greenhouse gas emissions and addressing the risks of global warming. This article explores the potential connections between the decarbonization of transport and oral health, highlighting the need for further research in this area. Emissions from vehicle exhausts, such as carbon dioxide, methane, and nitrous oxide, may have a modest impact on the risk of early childhood caries and other oral health diseases like periodontal diseases, oral cancer, and dental caries. Active transportation, which promotes regular exercise, has beneficial effects on overall health, including stimulating salivary protein production and reducing the risk of diabetes and cardiovascular diseases, both of which are linked to poor oral health. Transitioning to electric vehicles can also reduce noise pollution, positively impacting mental well-being, which is associated with improved oral hygiene practices. Furthermore, the development of sustainable infrastructure, including efficient public transportation systems, can enhance access to dental services. Further research is needed to establish stronger evidence for these connections and to explore how the global decarbonization of transport agenda can incorporate oral health considerations.
Full article
Open AccessCase Report
Assessment of Blood Glucose Responses in a Female National-Level Marathon Runner Using Continuous Glucose Monitoring during a Real-World Marathon Race
by
Fuminori Takayama
BioMed 2023, 3(3), 387-391; https://doi.org/10.3390/biomed3030031 - 27 Jul 2023
Abstract
►▼
Show Figures
Background: The effects of the use of continuous glucose monitoring (CGM) in elite endurance athletes are unclear. This case study reported the blood glucose (BG) levels of a female national-level marathon runner during a real-world marathon race. Methods: Heart rate and BG levels
[...] Read more.
Background: The effects of the use of continuous glucose monitoring (CGM) in elite endurance athletes are unclear. This case study reported the blood glucose (BG) levels of a female national-level marathon runner during a real-world marathon race. Methods: Heart rate and BG levels were monitored throughout the race. Results: The runner completed the race in 2:46 h:min, which was an improvement from her previous personal record by just under one min. Her BG levels were stable from approximately 5–40 km of the race at a mean concentration of 7.13 mmol/L, with a standard deviation of 0.20 mmol/L and a coefficient of variation of 2.8%. Increases in BG levels and heart rate were observed 6 min after the race and during the 40–42.195 km section, respectively. Conclusions: The runner broke her own record and exhibited stable BG levels throughout the race, with the highest BG value detected immediately after the race. Considering that quantity, content, and timing of pre-race meals and supplementation during the race can affect BG levels, future studies should assess additional detailed parameters in more detail and monitor multiple races with the same elite endurance athletes to acquire more definitive evidence on CGM usefulness among elite endurance athletes.
Full article

Figure 1
Open AccessArticle
Changing Responses during the COVID-19 Pandemic: A Comparison of Psychological Wellbeing and Work-Related Quality of Life of UK Health and Social Care Workers
by
Ruth D. Neill, Paula McFadden, Jill Manthorpe, John Mallett, Denise Currie, Heike Schroder, Jermaine Ravalier, Patricia Nicholl, John Moriarty, Susan McGrory, Rachel Naylor, Hannah Davies and Justin MacLochlainn
BioMed 2023, 3(3), 369-386; https://doi.org/10.3390/biomed3030030 - 26 Jul 2023
Cited by 1
Abstract
Aim: to explore the psychological wellbeing and work-related quality of life amongst United Kingdom (UK) health and social care workers during the COVID-19 pandemic. Subject and methods: Health and social care professionals within nursing, midwifery, allied health professions, social care and social work
[...] Read more.
Aim: to explore the psychological wellbeing and work-related quality of life amongst United Kingdom (UK) health and social care workers during the COVID-19 pandemic. Subject and methods: Health and social care professionals within nursing, midwifery, allied health professions, social care and social work occupations working in the UK during the pandemic were recruited. Repeated cross-sectional online surveys were conducted during six time periods of the pandemic (May–July 2020, November–February 2021, May–July 2021, November 2021–February 2022, May–July 2022 and November 2022–February 2023). Results: Over 14,000 participants completed the surveys during the data collection periods. The findings revealed that over the pandemic, psychological wellbeing and work-related quality of life scores significantly decreased. Conclusions: The overall psychological wellbeing and work-related quality of life of health and social care workers during the COVID-19 pandemic significantly declined. Further research is warranted on the lasting impact of the pandemic on this workforce. The health and social care workforce needs support to prevent further deterioration and to rebuild its wellbeing and resilience.
Full article
Open AccessSystematic Review
A Scoping Review on Coping Strategies and Quality of Life of Stroke Caregivers: Often Underestimated Variables in Stroke Recovery Process?
by
Anna Tsiakiri, Pinelopi Vlotinou, Aikaterini Paschalidou, Christos Konstantinidis, Foteini Christidi, Dimitrios Tsiptsios, Georgia Detsaridou, Alexandra Petridou, Aimilios Gkantzios, Stella Karatzetzou, Konstantinos Tsamakis, Erasmia Giannakou, Maria Emmanouilidou, Konstantinos Vadikolias and Nikolaos Aggelousis
BioMed 2023, 3(3), 349-368; https://doi.org/10.3390/biomed3030029 - 18 Jul 2023
Cited by 3
Abstract
►▼
Show Figures
The purpose of the present study was to review all available work published within the last decade focusing on coping strategies in stroke caregivers and their impact on quality of Life (QoL) and psycho-emotional status. A literature search of two databases (MEDLINE, Scopus)
[...] Read more.
The purpose of the present study was to review all available work published within the last decade focusing on coping strategies in stroke caregivers and their impact on quality of Life (QoL) and psycho-emotional status. A literature search of two databases (MEDLINE, Scopus) was conducted to identify all relevant full-text English studies published between 2013–2023. Sixteen articles were traced and were finally included. Cognitive and behavioral coping strategies were beneficial for stroke caregivers’ and survivors’ QoL. The level of mutuality in the caregiver-survivor relationship was associated with the impact of depressive symptoms on caregivers’ QoL and the protective effect of mutuality on survivors’ QoL over time. The level and quality of social support were positively associated with QoL for stroke caregivers and survivors. Caregivers’ preparedness was a moderator for the impact of depression on both caregivers’ and survivors’ QoL. High levels of spirituality had a significant role in ameliorating the negative impact of depressive symptoms on the psychological and physical QoL of stroke caregivers and survivors. In conclusion, the study of coping strategies can be used as a psychological reserve in the process of stroke rehabilitation and actively contribute to improving the QoL of both caregivers and stroke survivors.
Full article
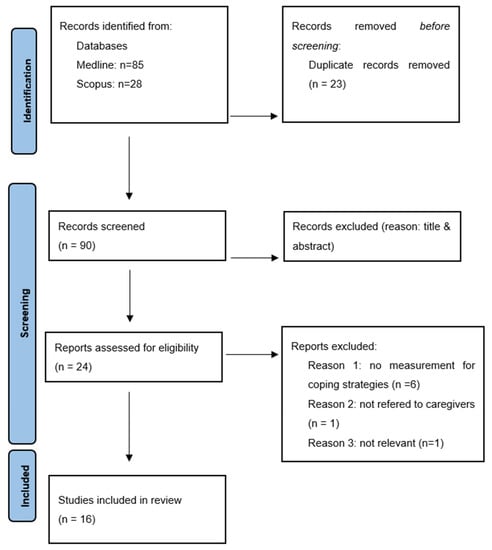
Figure 1
Highly Accessed Articles
Latest Books
E-Mail Alert
News
Topics
Topic in
BioMed, Biomedicines, Osteology, Pharmaceuticals, Pharmaceutics
Recent Advancement in Biotechnology and Drug Development Using Cutting-Edge Platforms
Topic Editors: Hani Al-Salami, Armin MooranianDeadline: 31 May 2024
Topic in
Biology, BioMed, Cells, Genes
Applications of the Zebrafish Model
Topic Editors: De-Li Shi, Pengfei XuDeadline: 30 June 2024
Topic in
BioMed, Biomedicines, CIMB, Foods, Nutrients
Novel Therapeutic Nutrient Molecules, 2nd Volume
Topic Editors: Sathish Kumar Natarajan, Jiujiu Yu, Corrine K Hanson, Melissa ThoeneDeadline: 31 December 2024





